|
A recent Canadian multi-centre retrospective study reviewed the baseline characteristics of critically ill patients with cirrhosis admitted to the ICU who underwent LT, although rates of graft failure were not available. Generalizing the US experience to Canadian centres may not be entirely appropriate, and studies of outcomes at Canadian centres with respect to this important issue are needed. The Canadian health care system differs from that of the United States, which may affect the availability of resources. There is sparse published Canadian evidence of the post-transplant outcomes of LT recipients with high versus low MELD scores. The authors found that these patients had inferior long-term graft survival ( p < 0.001) and patient survival ( p < 0.001) compared with patients with lower MELD scores however, their outcomes were deemed to be acceptable. In 2015, Panchal and colleagues 10 published the first US national multicentre outcomes report on patients with MELD scores of 40 and above undergoing LT. 7, 8 Over the last decade the frequency with which patients with high MELD scores have undergone LT has increased, and with limited organ supply it will probably continue to increase. Despite the MELD score’s important prognostic utility in predicting wait-list mortality, it is generally believed that it cannot predict post-transplant survival. 5 Patients with MELD scores of 40 or above have an estimated 3-month wait-list mortality risk greater than 70%, 6 and in practice these patients ultimately do not survive if they do not receive a transplant. 4 Subsequently, it has been validated as an accurate 3-month predictor of wait-list survival for potential LT recipients. The MELD score was initially introduced to estimate 3-month survival for patients with end-stage liver disease (ESLD) awaiting a transjugular intrahepatic portosystemic shunt (TIPS) procedure. 3 An advantage of the MELD score over alternative scoring systems is that the points derived from the MELD score are strictly objective (international normalized ratio, bilirubin and creatinine) whereas the Child–Pugh–Turcotte (CPT) score incorporates subjective assessments of hepatic encephalopathy and the amount of ascites (i.e., it essentially provides a nonobjective opinion of what is classified as mild, moderate and severe). 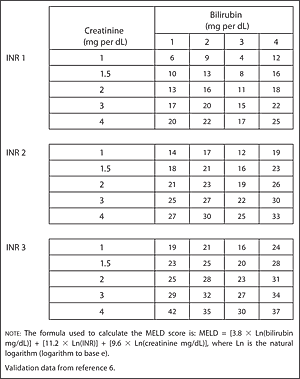
3 Before the adoption of MELD, they primarily used the CanWAIT ranking system, which ranks patients by location (at home, in hospital, in the intensive care unit or intubated in the ICU). 1, 2 In 2004, provinces in Canada began to adopt the MELD score for organ allocation. 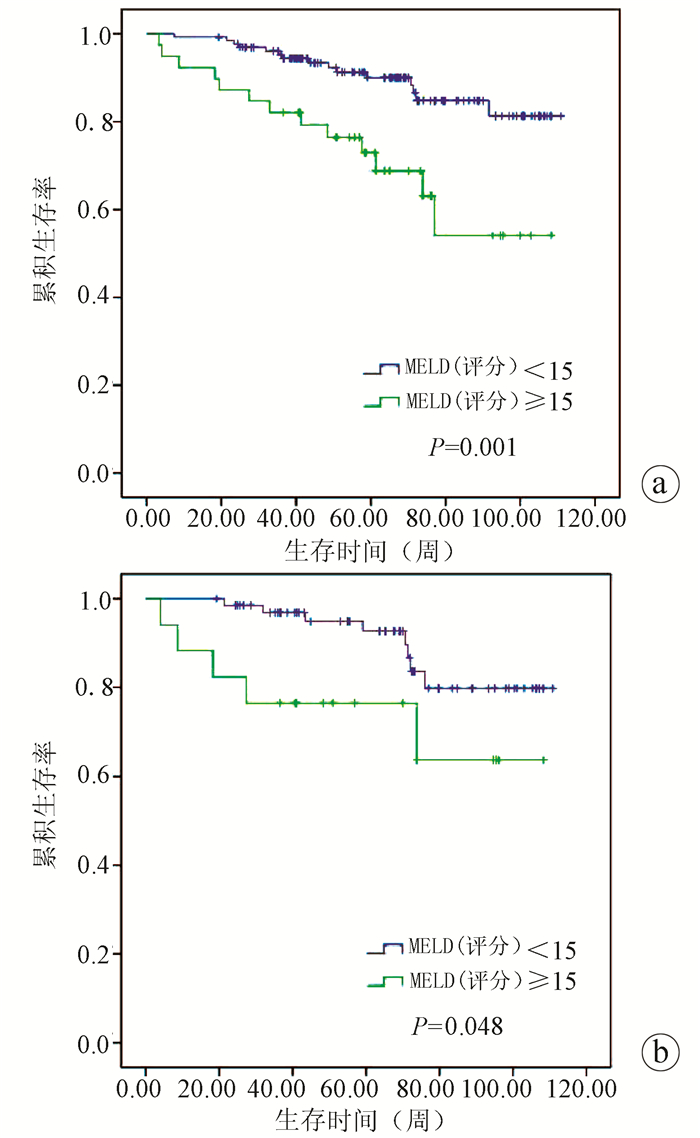
In 2002, the United States introduced the Model for End-Stage Liver Disease (MELD) score as an organ allocation tool to help prioritize liver transplant (LT) candidates on LT wait lists. D-MELD may potentially be used as an adjunct in determining risk of graft failure in recipients with high MELD scores. Graft survival was significantly lower in recipients with MELD scores above 35. When MELD was replaced with D-MELD (donor age × recipient MELD), it predicted graft failure but not patient survival.Ĭonclusion: No difference in patient mortality was found between MELD groups. Prior liver transplant was an independent predictor of patient mortality, and no independent predictors of graft failure were identified. One- and 3-year graft survival in recipients with MELD scores of 35 or lower was 91.7% and 90.9% versus 77.2% and 72.8% in recipients with MELD scores above 35 ( p < 0.001). One- and 3-year patient survival in recipients with MELD scores of 35 or lower was 93.1% and 84.9% versus 85.0% and 80.0% in recipients with MELD scores above 35 ( p = 0.37). 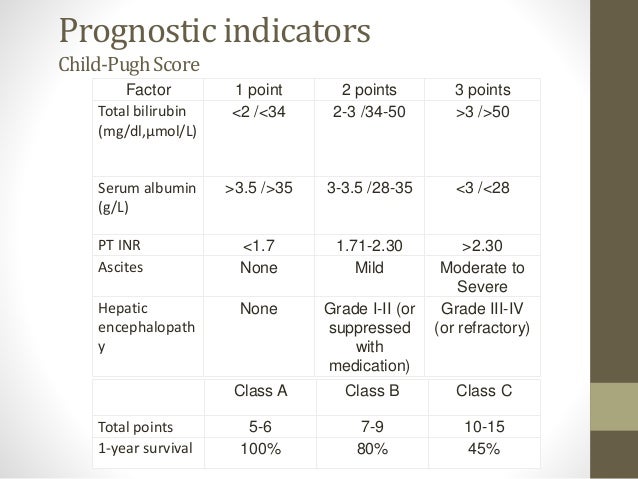
Patients with high MELD scores had higher rates of pretransplant acute kidney injury and dialysis ( p < 0.001), admission to the intensive care unit (ICU) or intubation ( p < 0.001), intraoperative blood product transfusions ( p < 0.001) and post-transplantation acute kidney injury and dialysis ( p < 0.001), as well as longer ICU ( p < 0.001) and hospital stays ( p = 0.002). Results: A total of 332 patients were included in the study: 280 patients had a MELD score of 35 or lower, and 52 had a MELD score above 35.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
